Treatments
The following medical information does not constitute professional medical advice. If you have any specific questions about any medical matter, you should consult your doctor or professional healthcare providers.
How is dry eye disease managed?
There are two main types of dry eye disease:
- Lack of watery tears
- Rapid tear evaporation due to lack of oily tears
The first step is to evaluate which type of dry eye is present; both types can be present at the same time.
The second step is to identify and treat or remove any underlying causes. You may be asked to stop certain medications, use a different type of glaucoma eye drop, use a different type of contact lens or reduce the number of hours you wear contact lenses.
The next step is to treat each type of dry eye in turn.
What can I do about dry eye disease?
There are several things you can do yourself to help improve tear production, reduce evaporation and reduce the symptoms of dry eye.
- Drink lots of water, as this helps improve tear production
- Get enough sleep each night
- Avoid alcohol or spicy foods, as these can cause meibomian oil gland blockage
- Avoid smoking or smoky areas as this makes the eyes drier
- Wear glasses or sunglasses on windy days to protect your eyes from the wind
- Avoid air-conditioned environments and draughts near your face, and consider using a humidifier to put more water into the air
- Remember to blink more frequently when using a computer screen or reading, and close your eyes or look away from the screen for a break every 30 minutes
What are the treatments for dry eye disease?
There are several different options your optometrist or ophthalmologist may suggest for treatment of your dry eye disease, depending on the type and severity of your condition.
Tear replacement
Artificial tears are eye drops used as a replacement for watery tears. Gels and ointments are also available, and are thicker than eye drops. They usually last longer in the eye and need to be put in less frequently, but can blur the vision.
There are many different types of artificial tears available without prescription. Preservative-free eye drops are recommended for use with contact lenses, or if they are needed more than four times a day.
Expressing natural oily tears to the ocular surface by daily hot eyelid massage can reduce the frequency of artificial tear drops required.
Switching to preservative-free glaucoma eye drops is recommended for patients with glaucoma who also have dry eye disease.1
Reduction of inflammation
Steroid eye drops or cyclosporine eye drops may be prescribed by an ophthalmologist if the dry eye condition has led to inflammation of the surface of the eye.
Prevention of tear drainage
When there is lack of watery (aqueous) tears, punctal plugs can be inserted into the tear duct (puncta) to stop tears from draining away and keep them on the surface of the eye for longer. They should be inserted by an optometrist or ophthalmologist. If the plugs help your dry eye but fall out, then punctal cautery can be considered. This is a simple procedure where the opening of the tear drainage tube is permanently sealed.
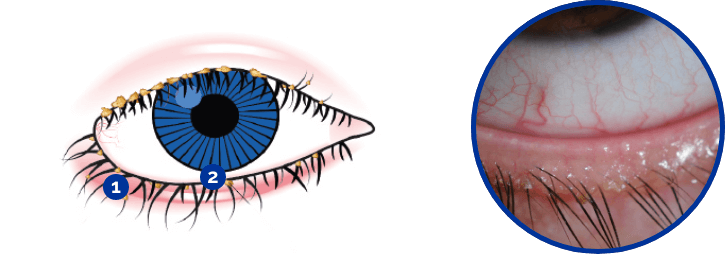
-
Eyelid swollen and reddened
-
Waxy material
What is meibomian gland dysfunction?
Blockage of meibomian oil glands in the eyelids, known as meibomian gland dysfunction, is the most common cause of dry eye disease. This causes rapid tear evaporation due to lack of oily tears.
Inflammation of the eyelids associated with waxy debris on the eyelashes is known as blepharitis. In blepharitis, rather than producing clear oily tears, the meibomian oil glands are blocked with waxy solidified oil. The blockage of the oil glands leads to them becoming inflamed, causing a burning feeling in the eyelids, which is worse in the morning. The waxy material collects on the eyelashes, causing grittiness, stickiness and itching of the eyelids. There is also rapid tear evaporation due to lack of oily tears.
What causes oil gland dysfunction is not well understood and likely to be multifactorial. It is thought that microbiological changes lead to an increased melting temperature of the oily tears, leading to blockage of the meibomian glands. Lifestyle factors associated with meibomian gland dysfunction include lack of sleep, excessive stress, and in some people, drinking alcohol and eating spicy foods. Omega three fatty acids, available as tablet supplements, and eating oily fish such as salmon and sardines are suggested to help improve meibomian gland dysfunction. Long-term use of certain types of glaucoma eye drops seem to be more likely associated with oil gland blockage than others.
How is meibomian gland dysfunction treated?
A simple way to help restore meibomian oil gland function is to carry out hot eyelid compresses and gentle massage daily. This will help to unblock the meibomian oil glands and express natural oily tears onto the surface of the eye. As an alternative to a hot towel, commercially available eye masks can also be used, but may not work for everyone.
The waxy debris on the eyelashes can be removed using eyelash-cleaning wipes. Avoid using baby shampoo as this removes natural oils from the surface of the eyes. Once the oil glands are expressing clear oil every day, rather than being blocked with thick wax, there should no longer be any need to continue with eyelash-cleaning wipes. Clean eye make-up away carefully and have at least one or two make-up free days per week.
If meibomian gland dysfunction is severe and has caused damage to the eyelids it may be necessary to take a course of oral antibiotics. Artificial tear supplements, topical antibiotics and topical steroids may also be prescribed.

Heat a small, thin, folded towel with hot running water (as hot as you can tolerate) and place over the closed eyelids. This will melt the thick wax which is blocking the oil glands.
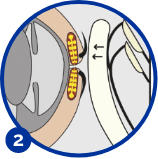
Push gently backwards on the upper eyelids for 10 seconds, near where the eyelashes come out. Try to squeeze the oil glands open gently, to express natural oily tears onto the eyeball.
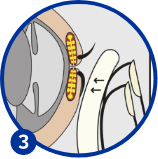
Reheat the towel in hot water and repeat the same movement on the lower eyelid for 10 seconds, towards where the eyelashes come out, to express oily tears on the surface of the eye.

Repeat again from Step 1, making sure to reheat the towel every 10 seconds.
Reference
- Stalmans et al. Eur J Ophthalmol 2013;23(4):518-525


